Collagen and Menopause: 8 Ways It Supports Your Body

Collagen and menopause are more connected than most women realize. As estrogen declines during perimenopause and post-menopause, collagen production drops with it — affecting your bones, joints, skin, sleep, hair, and gut simultaneously. If you are researching what collagen actually does during this transition, this guide covers all eight science-backed ways it supports your body, what the clinical research shows, and what to look for in a clean certified supplement.
✅ Direct Answer
Collagen production drops by as much as 30% in the first five years after menopause due to falling estrogen levels. Clinical research supports daily collagen peptide supplementation for eight key concerns during the menopausal transition: bone density, joint pain, skin integrity, body composition, sleep quality, hair thinning, gut lining health, and the perimenopause window. Consistent daily use at 5–15g is what the evidence supports.
Table of Contents
- Why Collagen Drops During Menopause
- Way #1 — Bone Density
- Way #2 — Joint Pain
- Way #3 — Skin Integrity
- Way #4 — Body Composition
- Way #5 — Sleep Quality
- Way #6 — Hair Thinning
- Way #7 — Gut Lining Integrity
- Way #8 — Starting in Perimenopause
- What to Look for in a Collagen Supplement
- How to Take Collagen During Menopause
- Simply Halal Collagen for Menopause
- Frequently Asked Questions
Why Collagen Drops During Menopause
Estrogen does more than regulate your cycle. It directly stimulates collagen-producing fibroblast cells in your skin and osteoblasts — the cells responsible for building new bone. When estrogen begins declining in perimenopause and drops sharply after menopause, collagen synthesis slows across your entire body at once.
Research shows women lose up to 30% of their skin collagen in the first five years after menopause, with an ongoing loss of approximately 2% per year thereafter. The same estrogen-collagen mechanism affects bones, cartilage, tendons, the gut lining, and hair follicles — all tissues that depend on collagen as their structural foundation.
This is not a cosmetic issue. It is a whole-body structural shift. Understanding this connection is why collagen supplementation during the menopausal transition has become one of the most studied areas in women’s health nutrition.
⚡ Quick Answer
Estrogen directly stimulates collagen production. When estrogen drops during perimenopause and menopause, collagen drops with it — affecting skin, bones, joints, gut lining, hair, and sleep simultaneously. Supplementing with hydrolyzed collagen peptides provides the raw amino acids your body needs to maintain these tissues when natural production slows.
Way #1 — Bone Density
This is where the evidence for collagen in menopausal women is strongest. A randomized, placebo-controlled trial published in Nutrients followed 131 postmenopausal women taking 5g of specific collagen peptides daily for 12 months. The collagen group showed significantly higher bone mineral density in both the lumbar spine and the femoral neck compared to placebo — with 4.2% higher BMD in the spine and 7.7% higher BMD in the femoral neck. The collagen group also showed increased levels of the bone formation marker P1NP, while the placebo group showed increased bone breakdown markers. (PubMed: 29337906)
A 4-year follow-up of this same cohort published in the Journal of Bone Metabolism found that continued collagen peptide supplementation produced further clinically relevant increases in spinal BMD — suggesting benefits compound with long-term consistent use. (PubMed: 34520654)
A 2025 meta-analysis in Frontiers in Nutrition reviewed 20 studies across 10 countries and found that collagen peptides — particularly combined with calcium and vitamin D — consistently improved bone mineral density at the spine and femoral neck in postmenopausal women across all four large RCTs reviewed. (PubMed: 41049371)
✅ Direct Answer
Multiple randomized controlled trials show that specific collagen peptides significantly improve bone mineral density in postmenopausal women at the spine and femoral neck — the two sites most vulnerable to osteoporotic fractures. Benefits are measurable at 12 months and increase further with continued long-term supplementation.
Way #2 — Joint Pain
Joint pain and stiffness is one of the most common symptoms of perimenopause — yet it is rarely discussed alongside hot flashes and sleep disruption. As estrogen declines, synovial fluid — the lubricant that cushions your joints — thins. Cartilage repair also slows because estrogen supports the cells responsible for maintaining cartilage structure.
Collagen peptides provide the three amino acids that cartilage and connective tissue are primarily built from: glycine, proline, and hydroxyproline. A 2024 randomized, double-blind, placebo-controlled trial in adults aged 45–65 with osteoarticular discomfort found that 24 weeks of hydrolyzed collagen supplementation improved body composition and neuromuscular performance, with particularly notable effects in women in the perimenopause and menopause range. (PMC: 12314484)
For a full breakdown of how collagen supports joint recovery and reduces pain, see our guide: Best Halal Bone Broth for Joint Pain and Recovery.
Way #3 — Skin Integrity
Skin thinning, increased dryness, and loss of elasticity are among the most visible effects of menopause-related collagen decline. The skin loses approximately 30% of its collagen in the first five years post-menopause, with an ongoing decline of 1–2% per year thereafter.
A 2019 systematic review in the Journal of Drugs in Dermatology found that oral collagen supplementation significantly improved skin hydration and elasticity across multiple clinical trials. (PubMed: 30681787)
Setting honest expectations matters here: results vary based on collagen source, dose, and consistency. What the research consistently supports is that hydrolyzed bovine collagen — taken daily at therapeutic doses — provides the amino acid building blocks skin cells need to maintain their structure when estrogen is no longer stimulating that production internally.
⚡ Quick Answer
Skin loses 30% of its collagen in the first five years after menopause. Daily hydrolyzed collagen supplementation provides the glycine, proline, and hydroxyproline your skin cells need to maintain elasticity, hydration, and structural integrity when estrogen is no longer driving that production.
Way #4 — Body Composition
Weight redistribution is a hallmark of the menopausal transition. Declining estrogen promotes increased visceral fat accumulation, reduced lean muscle mass, and a shift in how the body processes energy. This is not simply a calorie issue — it is hormonal and structural.
Research found that collagen hydrolysate supplementation in ovariectomized animal models — the standard preclinical model for menopause — significantly attenuated weight gain and adipocyte enlargement, suggesting a role for collagen in managing estrogen deficiency-related body composition changes. (PMC: 5118756)
In human trials, a 2024 RCT found that women in perimenopause and menopause taking hydrolyzed collagen alongside resistance training showed improvements in body composition including reduced fat proportion — an effect not seen in the placebo group. Collagen is not a weight loss supplement, but it supports the lean tissue maintenance that makes healthy body composition during menopause more achievable.
Way #5 — Sleep Quality
Sleep disruption is one of the most debilitating symptoms of the menopausal transition. Hot flashes interrupt sleep architecture, cortisol dysregulation delays sleep onset, and the drop in progesterone — a natural sedative — makes restorative sleep harder to achieve. What is less commonly discussed is how collagen addresses this from a nutritional angle.
Collagen is the richest dietary source of glycine — an amino acid with well-documented sleep-promoting properties. Research published in Frontiers in Neurology found that 3g of glycine taken before bedtime significantly improved subjective sleep quality, reduced daytime fatigue, and shortened the time to slow-wave sleep in people with sleep complaints. (PubMed: 22529837)
The mechanism is direct: glycine lowers core body temperature by increasing peripheral blood flow — and a drop in core body temperature is one of the key physiological signals that initiates sleep. For menopausal women whose thermoregulation is already disrupted by hot flashes, this cooling effect is particularly relevant. A single serving of Simply Halal’s Halal Collagen Bovine provides approximately 3g of glycine — the same dose used in the sleep research.
✅ Direct Answer
Collagen is the richest dietary source of glycine — clinically shown to improve sleep quality, reduce time to slow-wave sleep, and lower core body temperature. For menopausal women whose sleep is already disrupted by hot flashes and hormonal shifts, this glycine-sleep connection makes collagen before bed a practical, evidence-informed choice.
Way #6 — Hair Thinning
Hair thinning and loss is one of the most emotionally significant — and least discussed — symptoms of the menopausal transition. Research published in Maturitas confirms that estrogen decline directly impacts the hair follicle, which is an estrogen-sensitive tissue. As estrogen falls, follicles produce thinner and shorter strands, the growth phase shortens, and the rate of shedding increases. (PubMed: 40318238)
The collagen connection is structural. Hair follicles are housed in the dermis — the collagen-rich layer of skin. As dermal collagen thins after menopause, the structural support around each follicle weakens. A 2023 review published in Biomedicines described this as the hair follicle effectively “going through menopause” — with collagen loss in the dermal layer being a key mechanism behind reduced follicle performance during this transition. (PMC: 10669803)
A randomized controlled study in menopausal women found a statistically significant reduction in hair fall after three months of collagen supplementation compared to placebo, with the collagen group showing measurable improvement in follicle health markers. The researchers noted that collagen may enhance the synthesis of structural proteins in hair follicle cells — improving the dermal environment in which follicles operate during menopause. (MDPI: Nutrients 2025)
For a deeper look at collagen’s role in hair health, see: Halal Collagen for Hair, Skin & Nails — What the Science Says.
Way #7 — Gut Lining Integrity
Gut health changes during the menopausal transition in ways most women are not warned about. Declining estrogen affects the gut microbiome, increases intestinal permeability, and can contribute to bloating, digestive discomfort, and heightened inflammatory response — all of which are common perimenopausal complaints.
Collagen is uniquely positioned to support gut lining health because it is the primary structural protein of the intestinal wall. Its dominant amino acids — glycine, proline, and glutamine — are the exact building blocks required to maintain the tight junctions that keep the gut barrier intact. Research published in Food & Function found that collagen peptides significantly reduced intestinal epithelial barrier dysfunction by enhancing tight junction integrity in human cell models. (PubMed: 28174772)
A clinical study published in JMIR Formative Research found that daily collagen peptide supplementation reduced digestive symptoms including bloating, constipation, and intestinal pain in healthy women over an 8-week period. (PubMed: 35639457)
For menopausal women experiencing increased digestive sensitivity, supporting the gut lining with clean collagen daily is one of the most practical nutritional interventions available. The same grandmother’s wisdom that founded Simply Halal — that all disease begins in the gut — is now supported by a growing body of clinical evidence. Read our Our Story to understand why gut health has always been at the heart of this brand.
⚡ Quick Answer
Menopause affects gut microbiome diversity and increases intestinal permeability. Collagen’s amino acids — glycine, proline, and glutamine — are the structural building blocks of the intestinal wall and the tight junctions that keep it intact. Daily collagen supports gut barrier integrity during a transition that actively works against it.
Way #8 — Starting in Perimenopause
Starting collagen supplementation during perimenopause — the transitional phase that can begin 8–10 years before the final menstrual period — is likely more effective than waiting until after menopause. During perimenopause, estrogen levels fluctuate but haven’t yet dropped to their post-menopausal floor. Your collagen-producing cells are still active and responsive. Providing them with a consistent supply of the amino acids they need helps maintain production during the transition rather than trying to rebuild it afterward.
Think of it as structural maintenance versus structural repair. Both are valuable, but maintenance is easier. If you are in your 40s and experiencing irregular cycles, sleep disruption, joint stiffness, or skin changes — these are perimenopausal signals that your collagen architecture is beginning to shift. Starting a clean, consistent collagen protocol now builds the foundation before the steeper post-menopausal decline.
That said, the clinical research showing improved bone density was conducted in postmenopausal women — meaning it is never too late. The bone density trials showed measurable improvements at 12 months even in women with already-reduced BMD. The body retains the ability to respond to collagen peptide supplementation at every stage of the menopausal transition. The earlier you start, the more you preserve. But starting today is always better than waiting.
✅ Direct Answer
Start during perimenopause if possible — your collagen-producing cells are still active and more responsive to supplementation. If you are already post-menopausal, clinical trials show measurable benefits are still achievable. The best time to start is now, at whatever stage you are in.
What to Look for in a Collagen Supplement During Menopause
Not all collagen products deliver the benefits documented in clinical research. Source, processing method, and ingredient integrity all determine whether what is in the bag matches what is in the studies.
Grass-fed bovine. Type I and Type III collagen from grass-fed bovine sources are most relevant for menopause — covering bone, skin, gut, and connective tissue. This is the form used in the majority of clinical trials cited in this guide.
Hydrolyzed peptides. Collagen must be hydrolyzed to be properly absorbed. Non-hydrolyzed collagen passes through largely intact. Always check that the label says “hydrolyzed collagen peptides.”
No maltodextrin. Many commercial collagen powders use maltodextrin as a spray-drying carrier. It is a high-glycemic filler that contributes to gut inflammation — the opposite of what you want when supporting gut and bone health during menopause. For the full breakdown, read: Side Effects of Maltodextrin.
Third-party halal certification. ISA halal certification is not just a religious standard — it is third-party quality verification confirming animal source, processing facility cleanliness, and ingredient integrity. For a supplement you are taking daily for bone and joint health, knowing exactly what you are consuming matters. Read: Is Collagen Halal? Your Complete Guide.
How to Take Collagen During Menopause — Practical Protocol
Daily dose: 10–16g hydrolyzed collagen peptides. Bone density trials used 5g daily. Joint and skin trials typically use 10–15g. Simply Halal’s Halal Collagen Bovine provides 16g per serving — covering the full clinical range in one scoop.
Pair with Vitamin C. Vitamin C is a required cofactor for collagen synthesis. Taking collagen with a source of Vitamin C — citrus juice, berries, or a supplement — enhances your body’s ability to convert the peptides into new collagen fibers. This step is not optional for optimal results.
Take before bed for sleep benefits. To maximize the glycine-sleep connection, take your collagen 30–60 minutes before bedtime. Mixed into warm water or herbal tea it doubles as a calming evening ritual.
Combine with resistance training. Multiple trials show that collagen peptides combined with resistance exercise produce significantly better outcomes for body composition, lean muscle maintenance, and joint recovery than collagen alone. Even light resistance training 2–3 times per week amplifies the structural benefits.
Consistency above everything. Clinical research showing meaningful results runs 12–24 weeks minimum. Building collagen into a daily routine — morning coffee, smoothie, or warm water before bed — matters more than the exact timing.
For a full daily structure, see: Halal Collagen Daily Routine 2026.
Simply Halal Collagen for Menopause
Simply Halal was not built in a lab. It was built in a kitchen by a family that spent three years researching exactly what clean nutrition looks like — 160+ lab tests, partnerships with the MSU Product Center Innovation, and personal sourcing from grass-fed cattle in Argentina — before a single bag was sold.
Co-founder Fatima Hammoud healed her own chronic sinus infections in 2002 using homemade bone broth — without surgery or antibiotics. Her family has been allergy-free since. That healing story, rooted in the belief that all disease begins in the gut, is why gut and connective tissue health have always been at the center of everything Simply Halal makes.
Every product is ISA-certified, grass-fed, free from maltodextrin and artificial additives, and chef-crafted by Master Chef Maher Fawaz with 28 years of culinary and nutritional expertise. For women navigating perimenopause and menopause, it means a supplement you can verify, trust, and take every single day.
- Halal Collagen Bovine — 16g Type I & III hydrolyzed collagen per serving, grass-fed, ISA certified
- Halal Collagen Broth — 14g collagen with organic ingredients, chef-crafted
- Wellness Bundle — all three Simply Halal products at the best available price
Free shipping on bundles. Ships nationwide across the USA. For more on the science behind halal collagen peptides see: Halal Collagen Peptides: 7 Benefits for Skin, Hair & Joints. For the complete halal collagen guide: Halal Collagen: The Complete Guide 2026. For collagen specifically for women over 40: Collagen for Women Over 40: What the Science Actually Says.
Frequently Asked Questions — Collagen and Menopause
Does collagen help during menopause?
Yes. Clinical research supports collagen supplementation for eight key menopause-related concerns: bone density loss, joint pain, skin thinning, body composition changes, sleep disruption, hair thinning, gut lining integrity, and the perimenopause window. Benefits are most consistent with daily use at 5–15g for a minimum of 8–12 weeks.
Why does collagen drop during menopause?
Estrogen directly stimulates collagen synthesis in the skin, bones, and connective tissue. As estrogen declines during perimenopause and drops sharply after menopause, collagen production falls by as much as 30% in the first five years post-menopause.
Can collagen help with bone loss after menopause?
Yes. A randomized controlled trial published in Nutrients found that postmenopausal women taking specific collagen peptides for 12 months showed significantly higher bone mineral density in the spine and femoral neck compared to placebo. A 4-year follow-up showed continued BMD improvement. (PubMed: 29337906)
What type of collagen is best for menopause?
Type I and Type III bovine collagen are most relevant — covering bone, skin, gut, and connective tissue. Both are found in Simply Halal’s ISA-certified Halal Collagen Bovine — grass-fed, no maltodextrin, no fillers.
How much collagen should a menopausal woman take daily?
Clinical studies use 5g to 15g of hydrolyzed collagen peptides per day. For bone density, 5g daily is most cited. For joint, skin, and sleep benefits, 10–15g is more commonly studied. Simply Halal’s Halal Collagen Bovine provides 16g per serving — meeting the upper clinical threshold in one scoop.
Can collagen help with sleep during menopause?
Yes. Collagen is the richest dietary source of glycine — clinically shown to improve sleep quality, shorten time to slow-wave sleep, and lower core body temperature. Research in Frontiers in Neurology found 3g of glycine before bedtime significantly improved sleep in people with sleep complaints. (PubMed: 22529837)
Does collagen help with menopausal hair thinning?
Yes. Hair follicles are housed in the collagen-rich dermal layer of skin. As estrogen declines, dermal collagen thins and follicle support weakens. A randomized controlled study in menopausal women found statistically significant reduction in hair fall after three months of collagen supplementation versus placebo.
When should I start taking collagen for menopause?
Starting during perimenopause is more effective than waiting — your collagen-producing cells are still active and more responsive. That said, clinical trials showing bone density benefits were conducted in postmenopausal women, so it is never too late. Start at whatever stage you are in.
You might also like

24 May 2026
Best Halal Bone Broth Powder for Athletes
Athletes put more stress on connective tissue than any other population. Every training session

4 May 2026
Best Halal Bone Broth Powder for Skin
Skin health supplements are one of the most crowded categories in the wellness market.

3 May 2026
Best Halal Bone Broth Powder for Keto
If you are on a ketogenic or low-carb diet, bone broth powder is one

2 May 2026
Best Halal Bone Broth Powder for Joints
Joint pain is one of those problems that announces itself slowly. A knee that

2 May 2026
Best Halal Bone Broth Powder for Weight Loss
The bone broth and weight loss space is full of dramatic claims. Detox diets.

2 May 2026
Best Halal Bone Broth Powder for Gut Health
Most people treat gut problems as symptom problems. They reach for antacids when they

29 Apr 2026
Halal Collagen Powder vs Bone Broth Powder: Which One Is Right for You?
Two questions Simply Halal customers ask before buying: what is the difference between halal
26 Apr 2026
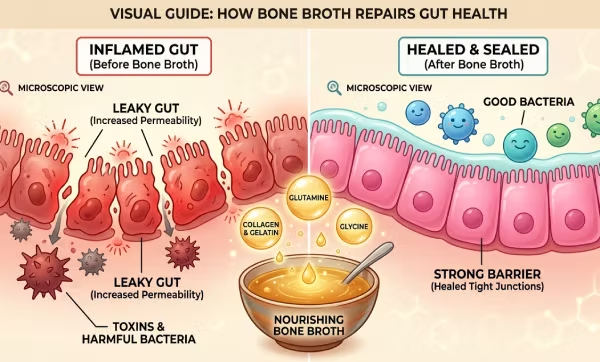
Best Halal Bone Broth for Gut Health: 5 Powerful Science-Backed Benefits
✅ The Simply Halal Origin Story Co-founder Fatima Hammoud’s grandmother told her something modern

25 Apr 2026
Halal Bone Broth Powder vs Stock Cubes: What’s the Difference?
✅ The Short Answer Stock cubes are dehydrated seasoning products — typically 40-60% salt

25 Apr 2026
How to Use Halal Bone Broth Powder for Cooking: 8 Everyday Uses
Halal bone broth powder for cooking is one of the most versatile ingredients you
